Safe Injection Sites (also known as SCF’s or Safe Consumption Facilities along with MSIC’s or Medically Supervised Injection Centers) are locations (usually state/federal funded or non-profit) that allow people who use drugs to safely inject them with sterilized equipment under the supervision of caring and clinically trained staff. These facilities are usually staffed with medical professionals and have access to opioid overdose preventative medication such as naloxone, along with first aid equipment, healthcare educational material, and referrals for addiction treatment centers nearby. In a study compiled in 2014 on SCF’s in Europe, the majority of facilities were found to provide the following services:
- Syringes/Paraphernalia
- Healthcare Education Materials/Resources
- Bread, Coffee/Tea
- Treatment Referral
- Phone access/charger
- Shower/washing machine
- Social support
- Warm meals
- Registered Nurses
- Work Referral
- Doctor
- Lockers
The first safe injection facility was opened in Switzerland in 1986. Further sites were developed throughout Europe in the 90’s and 2000’s. Today, there are roughly 100 supervised injection facilities in 66 cities in 11 countries around the world, including in:
- Germany
- Spain
- Netherlands
- Norway
- Luxembourg
- Switzerland
- Denmark
- Canada
- Australia
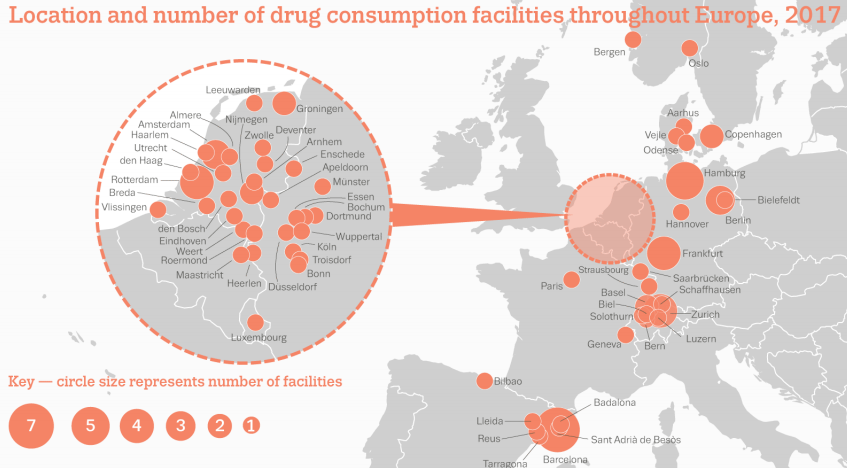
Courtesy the European Monitoring Centre for Drugs and Drug Addiction
Types of Safe Injection Facilities
Safe Injection Sites come in many different sizes and varieties. Each one may run according to a different organizational and staffing model. The three basic models of SIF’s are Integrated, Specialized, and Mobile.
Integrated
Integrated facilities are the most common type of SCF. This facility type houses multiple services, including shower and laundry facilities, counseling and blood testing services, needle and syringe exchanges, psychosocial care, employment programs, medical services, and referral resources.
Specialized
Specialized SCF’s are those that are part of a larger organization. They are typically in close proximity to a drug treatment center or high drug traffic area, and are singularly focused on providing an environment to safely consume drugs in. These SCF’s do not have all the benefits of an integrated facility.
Mobile
Mobile facilities are vans outfitted with injection booths offering a limited range of services such as needle and syringe exchange, blood testing, and referral services. These have the least amount of capabilities but offer the ability to cover a greater range.
Pros of Safe Injection Sites
Proponents of safe injection sites say that you can’t force people to stop taking drugs, whether that be through criminalizing possession, harsh consequences, or simply telling them to stop. Therefore, it’s best to offer drug users a safe way to inject these drugs and minimize their risk of contracting a disease or overdosing. It humanizes drug addicts and provides an alternative to the “War on Drugs” mentality.
Unfortunately, while the majority of SCF’s are located in Europe, we have a dearth of knowledge when it comes to how effective these facilities are. The biggest studies we have come from facilities in Vancouver, Canada, and Sydney, Australia. Based on collected evidence gathered from studies over the past twenty years, there are a number of measurable benefits to these programs along with more nebulous statistics that will require better research methodologies for future implementation.
Data compiled from Philadelphia based report on Supervised Consumption Facilities from December 2017 and data from the Massachusetts Task Force on Opioid Therapy and Physician Communication published in April of 2017.
Reduction in number of overdose deaths
Multiple studies of supervised consumption facilities (SCF’s) show that they reduce the number of fatal overdoses in their regions. For example, in a study on an SCF facility in Vancouver, Canada researchers documented a 35% reduction in mortality within 500 meters of the facility within three years of opening. Another study in Spain showed that overdose deaths were halved from 1991 to 2008. A similar study in Sydney, Australia showed that ambulance calls for opioid-related overdoses decreased by 68% during the times the facility was open.
Reduction in unsafe injection practices
There is no evidence that the total number of HIV infections in the area is reduced. However, evidence from both the SCF’s in Vancouver and Sydney have shown a reduction in the number of new HIV infections. This is because in all locations the facilities are only able to serve a small percentage of the population. In Vancouver, researchers estimated that the clinic prevented more than 80 HIV infections annually, resulting in annual savings of about $13.7 million in HIV medical care. Evidence from Spain showed a reduction in new HIV infections from 19% to 8.2% from 2004 to 2008. In 45 studies carried out in Europe, the majority showed a positive relationship between SCF’s and HIV prevention. Currently, the mortality rate for intravenous drug users is eight times higher than the rest of the population. By reducing the risk of overdose and risk of infection, this number could be lowered. Plus all, studies have shown that attendees significantly reduce their engagement in unsafe injection methods.
Reduced Healthcare Costs
There have been no definitive studies on the exact relationship between health care cost savings associated with SCF’s, but multiple theoretical studies by cities have predicted considerable savings based on mathematical models. In Vancouver, the savings were estimated at $13.7 million annually. Proposals in Philadelphia, Maryland, and San Francisco all predict cost savings returns from SCFs.
Increase in Treatment Referrals
In Vancouver, the Safe Consumption Facility was associated with increased rates of referral to addiction care centers, increased detox facility referrals, and more methadone clinic referrals. Enrollment in all of these facilities raised by an average of 30%. In Vancouver, studies found that there was no statistically significant increase or decrease in the number of local people injecting drugs. In other words, the sites don’t decrease or increase the number of addicts, but they do get more people in treatment.
Cons of Safe Injection Sites
Detractors believe that opening these kinds of sites will not only attract more drug users to the neighborhoods they open up in, but will also encourage greater drug usage among addicts. By removing the barrier, and the stigma, to drug use, states will be actively encouraging harmful drug usage using taxpayer money. When Vermont proposed introducing safe injection sites, the federal Justice Department intervened and argued that the facilities threatened to “undercut existing and future prevention initiatives” in the state.
Increase in Public Drug Usage/Crime
Detractors typically assume that safe injection sites will naturally draw more drug users, and therefore increase rates of drug use and associated crime to the neighborhood where it is located.
FALSE
The vast majority of studies from Europe, Canada, and Australia have demonstrated that public consumption decreases in the surrounding areas where facilities are located. In Sydney, no evidence was found that the existence of the facility led to either an increase or a decrease in thefts or robberies around the facility. In Vancouver, there was no increase or decrease in the number of charges associated with drug trafficking, including assaults and robbery. Leftover needles and public consumption in Vancouver was reduced by roughly 50%.
Safe Injection in the United States
Several big cities throughout the U.S. have been considering opening facilities for safe injection, including New York, San Francisco, Philadelphia, and Seattle. In May of this year, for example, New York City Mayor Bill De Blasio stated that he plans to open the city to supervised drug consumption facilities and safe injection sites. Dubbed “Overdose Prevention Centers,” these facilities would need to pass approval from district attorneys and the state Health Department before they could open. The cities currently considering legislation to legalize SCF’s are:
- New York
- Montpelier
- San Francisco
- Philadelphia
- Seattle
- Denver
- Ithaca
- Massachusetts
The biggest barriers to adoption remain public approval and legal jurisdiction. For the latter, states would need to apply for federal exemption from the Controlled Substances Act to designate how much of a substance would be legally allowed. The question of professional liability concerning health issues and possible overdose is also complicated. To what degree will physicians be held responsible for negative outcomes? Similarly, achieving approval from public opinion, especially from law enforcement, will be necessary to integrate the facilities successfully.
The Underground Injection Railroad
While no American states have received approval to create public safe injection sites, there has been a growing population of underground injection facilities. One, opening in late 2014, has been operating and documenting their progress swaddled in anonymity. After more than two years of observation, addiction researchers Alex Kral and Peter Davidson are advocating for a large-scale adoption based on promising results from what has been dubbed the “Underground Safe Injection Site.”
The nonprofit group has been operating on a budget of $150,000 a year, and hopes to see their research promoted in the widespread adoption of Safe Injection Sites throughout the rest of the U.S. So far, research has shown that the facility has had the same positive outcomes reported by past studies, such as reduction in overdose deaths, reduced unsafe injections, and less public drug consumption.
An unexpected side benefit of the facility is that patients and staff members have experienced a greater degree of community because of the underground nature of the operation. The significant legal, financial, and career risks undertaken by the facilitators has endeared them even more to the addicts they are serving. Addicts are also encouraged to share their experiences through anonymous tablet-computer surveys, allowing feedback to influence the development of the program and provide insight into the less quantitative benefits that the program could be creating.
‘The main argument I hear against them is that if you open one of these, it is the government condoning drug injection, and people will think using drugs is okay. These sites have not increased drug use, nor made drugs more attractive to anyone else, but have had all these positive effects, including keeping users from doing drugs in front of you and your kids on the street. We’ve been saying that drugs are bad since Nixon, and 40 years later, more Americans are dying from drug overdose and abuse than ever in our history.’ – Peter Davidson, Ph.D. Addiction Specialist.
How to Implement Safe Consumption Facilities
This approach is based on the Massachusetts State Task Force on Opioid Therapy and Physician Communication Task Force. These guidelines are derived from a compilation of the majority of available and significant studies on the subject of Safe Consumption Facilities.
- Apply for an exemption from federal drug laws to implement a pilot SCF program and pursue state legislation legalizing the program, working in tandem with other states pursuing similar legislation
- Create an advisory board of experts that includes experts from the SIF (Supervised Injection Facility) in Vancouver, and the MSIC (Medically Supervised Injecting Center) in Sydney Australia, along with state and federal officials under the jurisdiction of a task force, to design the evaluation protocol (including careful design of informed consent protocols regarding research) for the pilot program.
- Utilize program information from the underground safe injection sites and, if possible, onboard administrators to oversee correct methods of implementation for the program.
- Consider implementing multiple harm-reduction strategies (counseling, referral, and placement for all types of drug treatment) as a component of the pilot to ensure comprehensive health care is available to all marginalized persons who inject drugs. This could be achievable by partnering with reputable local treatment centers.
At Landmark Recovery, we are continually advocating for evidence-based treatment methods. The correct way to combat addiction is to address it with the complexity it requires, entailing holistic treatment options from drug and alcohol recovery centers that may seem out of the box but that get results.
In Conclusion
Safe Consumption Facilities are not the cure, but they are the right step in a direction towards healing communities riddled with addiction. Users don’t enter SCF’s to treat addiction, but they do receive services and assistance that are proven to help with a number of key issues. These include: reducing the risk of transmission of human immunodeficiency virus (HIV) hepatitis B and C (HCV), decreasing the number of fatal overdoses, minimizing public nuisances caused by drug use such as public drug usage and leftover needles, and improving access and enrollment in health and social services.
U.S. Surgeon General Dr. Jerome Adams recently proclaimed support for supervised injection facilities and other evidence-based treatment methods. Speaking at the American College of Physicians in Washington D.C., Adams referenced the statistics and applauded numerous states such as Denver, Philadelphia, San Francisco, and New York for taking steps towards legalizing these facilities. Another sign of their success is that these programs have been ongoing in other countries for over two decades, and they continue to receive support, funding, research while they have been steadily expanding.

Choose Recovery Over Addiction
We're here 24/7 to help you get the care you need to live life on your terms, without drugs or alcohol. Talk to our recovery specialists today and learn about our integrated treatment programs.



